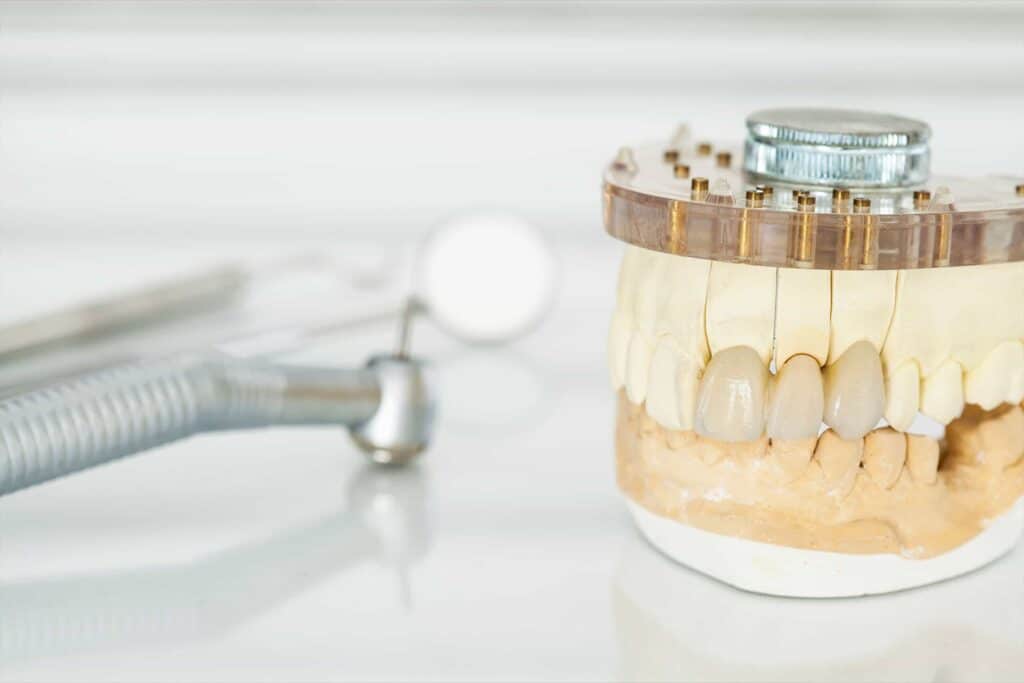
Dental crowns, along with dental fillings, are some of the most common dental treatments rendered every year. In fact, there is a good chance that you have one yourself! Crowns are very common and are considered by dentists to be a basic but necessary procedure. Crowns are completed for various reasons, but a primary purpose is to protect the underlying tooth from fracture. This can significantly increase the longevity of the tooth amongst other positives.
What Are Dental Crowns?
Dental crowns are a type of prosthesisAn artificial body part, which is often lost due to disease or trauma. that typically covers the entire tooth. The primary purpose of dental crowns primary is to protect the underlying tooth. Imagine they’re like a hardhat; if a brick falls on a construction worker’s head, the hardhat will take the brunt of the force and prevent a trip to the hospital. This helps to prevent a fracture that could result in a root canal or extraction. Additionally they can also improve the esthetics of a tooth by giving it the ideal shape, size, contour, and color.
Dental crowns are utilized for many reasons, and often it’s due to a combination. Instances where dental crowns are used include to fix a severely worn or broken tooth, a weak tooth due to tooth decay or a large filling, gaps between teeth causing food impactionWhen food gets stuck in between teeth. This causes irritation in the gums and can be very uncomfortable., or esthetics.
There are multiple types of dental crowns and they can be made up of different types of materials. There are some types that do not cover the entire surface, such as onlay and inlay. These are commonly referred to as a partial crown, which as the name implies, partially covers the tooth. There are also other styles of crowns that don’t encompass the entire tooth such as a ¾ (three quarters) crown.
There are several advantages to partially covering a tooth, with the primary one being you save tooth structure. Once part of a tooth is lost for any reason, including decay, trauma, or when restoring a tooth, you never get that tooth structure back. However removing of some of the natural tooth in order to place a crown can be the best option for longevity.
What Are Crowns Made Of?
As far as materials are considered, there are several different types of dental materials used for dental crowns. The most common materials used for the different types of dental crowns include ceramic, also known as porcelain, gold alloyA mixture of metals that aims to blend the best properties of each metal. Gold crowns are not 100% gold, but contain other metals such as platinum, palladium, silver, copper or tin., and resin. A vast majority of crowns are metal crowns or porcelain crowns, or a combination of the two. However there are circumstances when resin crowns are made.
There are also different types of ceramic crowns and different compositions of gold used for crowns as well. A few common types of porcelain crowns include feldspathic porcelain, leucite reinforced pressable porcelain, lithium disilicate, and zirconia. Stainless steel is also used, but is primarily used for children.
Ceramic or Porcelain Crowns
Used interchangeably, ceramic and porcelain crowns are perhaps the most common type of crown used today. As technology improves, ceramics are becoming more mainstream as the material of choice for dental crowns due to better aesthetics, inertness, biocompatibility1https://www.sciencedirect.com/science/article/abs/pii/S0142961203007907. Many patients express satisfaction with all ceramic crowns2https://www.sciencedirect.com/science/article/abs/pii/S0022391300700333.
Additionally modern day ceramic crowns have excellent physical properties including good marginal adaptation3https://www.sciencedirect.com/science/article/abs/pii/S0022391313001868, which is key in the longevity of crowns. Earlier versions of all ceramic crowns saw more failures due to the inherent brittleness of the material itself1https://www.sciencedirect.com/science/article/abs/pii/S0142961203007907. Current research aims to improve clinical outcomes by understanding how variables such as the elastic modulus, hardness, strength, and toughness affects fracture mechanics1https://www.sciencedirect.com/science/article/abs/pii/S0142961203007907.
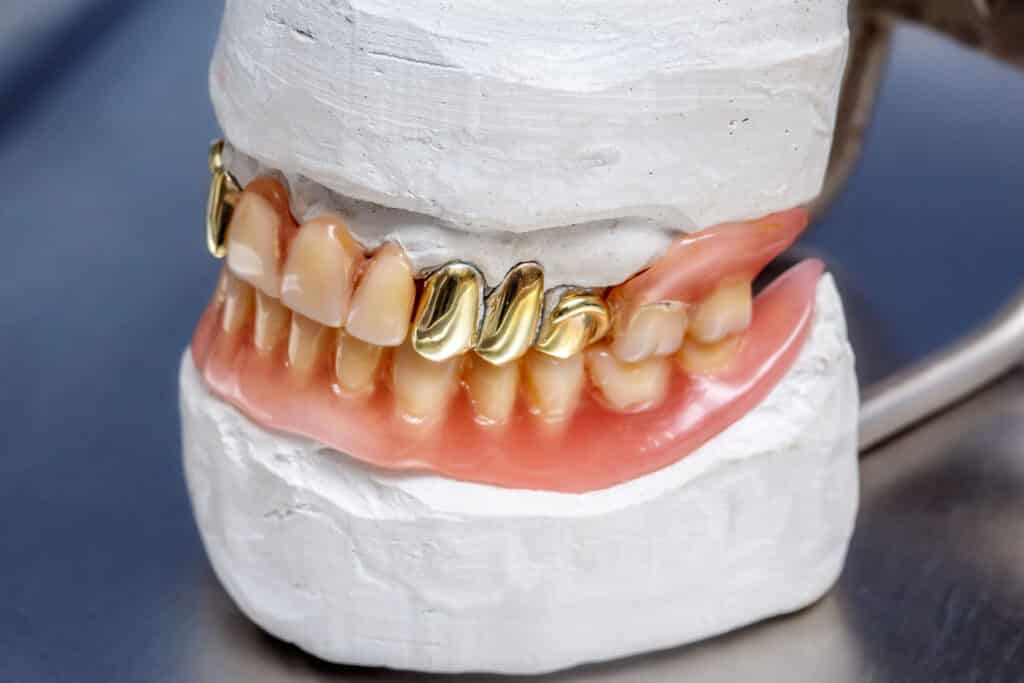
Gold Crowns
Gold has many superior physical properties that, except for esthetics, make it an ideal crown material. It has good physical, chemical, mechanical and biological properties. A gold crown is almost never made of 100% gold since a combination of multiple metals optimizes the aforementioned properties. For example, if a crown was made from pure gold, it would deform easily during routine eating due to the gold itself being soft (HV 25), having low stress proof (30MPa) and large elongation (45%)4https://link.springer.com/content/pdf/10.1007/BF03215496.pdf.
That deformation could open up the marginThe interface between a restoration and the tooth. This is the most common area for a cavity to reoccur on a tooth. and lead to recurrent cariesDental caries that reoccurs at the margin of an existing restoration.. While there are several instances where gold crowns have a higher gold content such as gold fillings, they are rarely completed today due to the cost and complexity of treatment.
Metallic crowns have seen a decline in recent years even to the point where there are dental labs that do not make gold crowns. Due to the rising cost of gold and esthetics, gold crowns will be used less frequently however they will still be used due to their longstanding history as permanent crowns.
Porcelain Fused to Metal Crowns (PFM)
Porcelain fused to metal crowns were once an extremely popular type of dental crown. As the name implies, this style of dental crown utilizes a metal substructure that has porcelain baked onto the metal. The idea behind porcelain fused to metal dental crowns are to blend the best properties between a ceramic crown and metal crown.
However recent dental crown materials, in particular zirconia crowns, have better strength and esthetics than porcelain fused to metal crowns. As technology and research increases, porcelain fused to metal crowns may no longer be used.
Resin Crowns
Resin dental crowns are functionally the same as the other types of dental crowns, however they are made of resin instead of ceramic or metal. This type of dental crown is not done frequently due the poorer physical properties. In short resin crowns are weaker and less esthetic but can be used in a few circumstances. Due to this, ceramic crowns will continue to be the primary material used while metal or resin crowns used on occasion.
Stainless Steel Crowns
Stainless steel crowns (SSC) are a preformed crown indicated for pediatric use. Adults are rarely given a stainless steel crown due to it’s extremely poor physical properties. Since baby teeth will fall out, a permanent crown is not needed. Stainless steel crowns can be used for front and back teeth, however recently a preformed zirconia crown is also used for children.
Why or When Do I Need a Crown?
When there is a weak tooth that is susceptible to fracture, a dental crown is needed to protect the natural tooth from irreversible damage. Teeth are weakened due to a variety of reasons including: disease, trauma, or large amounts of filling material. On the other hand a crowned tooth is well protected from fracture and a permanent crown will increase the longevity of teeth significantly. Another reason are severely discolored teeth, which cannot be fixed with whitening. This is most common with tetracycline staining, but is a cosmetic reason for a dental crown.
The healing ability of teeth also plays a role. Natural teeth are unique bones that do not regenerate by themselves. If you were to fall down and fracture your arm, it will heal with proper treatment. If you were to fall down and break a tooth, that damaged tooth will not regenerate regardless of time or treatment. Our teeth, like our bodies, are susceptible to wear and tear, trauma, and disease that require treatment over time. Misuse, such as chewing ice, also increases the need for a traditional crown.
As diseased and broken teeth are treated with fillings, they are healthier but become weaker than a tooth that’s never been treated. Each time a filling is placed and replaced, the new filling is bigger than the previous and there is less remaining original tooth as well.
When Should I Consider Getting a Dental Crown?
As the fillings get bigger, the remaining tooth structure gets smaller and more susceptible to fracture. As a general rule of thumb, once the filling material covers more than 50% of the occlusalThe ‘top’ of teeth where chewing occurs on posterior teeth. This surface has pits and grooves. surface or a filling is more than 50% of the anatomical crownThe portion of the tooth from the dentinoenamel junction (DEJ) to the occlusal or incisal surface. Sometimes a portion is under the gums and not visible., one should start thinking about placing a crown on the tooth.
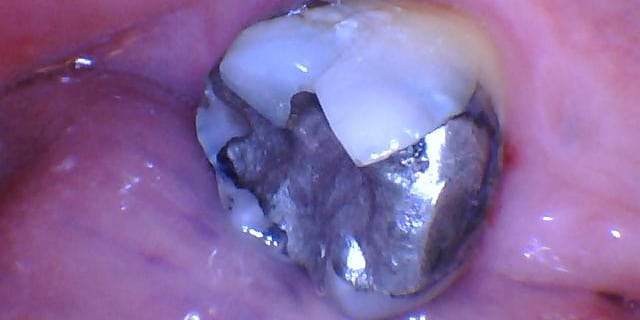
After tens of thousands of cycles of chewing, the vulnerable part of the tooth weakens and eventually breaks. How a damaged tooth breaks ultimately determines how and if the tooth can be fixed. Teeth will generally break in one of five ways:
- The fracture starts and ends above the gums without involving the nerve. This is the best case scenario and if the nerve is unaffected, it only requires a buildup and a crown. The newly crowned tooth has a good prognosisThe proposed treatment is the ideal treatment and is expected to last within the usual time frame. For instance if a small piece of tooth is fractured but is easily savable with a crown that is projected to last the expected 10-15 years, the tooth has a good prognosis. even after fracturing.
- The fracture starts and ends above the gums, but involves the nerve. This exposes the nerve and is extremely painful. The tooth can be saved, but needs root canal treatment in addition to a buildup or post and coreA small thin metal or fiber rod that is glued in the canal of a root canaled tooth. Its main purpose is to retain the core, which is a filling under a crown. and crown. This scenario still has a good prognosisAn estimation of the success and longevity of proposed treatment on a tooth, based on various clinical factors. In other words, how long will the tooth last before needing treatment again. and the tooth should be saved.
- The fracture starts above the gums but ends at or near the bone. The tooth can be saved here, however it would require a procedure called crown lengthening to avoid violating biologic widthA distance between the bone and where the gums attach to the teeth. This distance must be maintained to preserve good periodontal health.. Additionally the tooth needs a buildup and crown. Depending on the long term prognosisThe estimation of how long the proposed treatment will last. of the tooth, saving the tooth may not be the best option since bone is removed in order to save it.
- The fracture starts above the gums, ends at or near the bone, and involves the nerve. This requires crown lengthening, RCT, and a buildup and crown. While the tooth can be saved, the tooth will have a guarded prognosisThe proposed treatment is not expected to last the usual amount of time. It may still be a good option but the patient must understand that if the treatment fails within a shorter time frame, it is expected., and cost about the same as a dental implant. It is usually better to extract the tooth and replace it with an implant in this scenario.
- The fracture splits the tooth in half, often involving the nerve. The tooth cannot be saved in this scenario and must be removed and replaced with something such as a dental implant or dental bridge.
By placing a dental crown on a susceptible tooth prior to fracture, the health and future of the tooth is much more predictable. Since it is difficult to impossible to predict how a tooth will fracture, it is best to prevent all fractures and not wait until the tooth ultimately fractures. This is why many dental offices will recommend dental crowns on teeth that are asymptomatic – to prevent the previously mentioned 5 scenarios, but especially scenarios 3, 4, and 5.
Why Do Root Canaled Teeth Need a Crown?
Another reason a tooth needs a dental crown is if it’s had root canal treatment. The neurovascular bundleA structure that has a combination of two or more of nerves, veins, arteries, and lymphatic vessels traveling in tandem. contains vessels that give vitality to the tooth itself. Once removed during a root canal, the tooth becomes very brittle and requires a dental crown procedure to protect it from fracture.
Root canaled teeth without a protective crown can break in as little as a few months, sometimes badly enough to require extraction. Thus in order to ensure root canaled teeth will last as long as possible, they need crowns. Unlike the posterior teeth, anterior teeth do not always need to be crowned after a root canal. It is only when it has large fillings, does a root canaled anterior tooth need a dental crown, most often an all porcelain crown.
What Are Some Other Symptoms That I Need a Dental Crown?
The previous reasons would be prior to any symptoms or fractures in the tooth. Once a tooth starts to hurt, it can mean more treatment is required than a dental crown or filling. Here are some symptoms that indicate when a tooth may need a permanent crown:
- The tooth or filling fractures
- Cracked tooth syndromeAn incomplete fracture that extends into the dentin and possibly further into the tooth. A classic symptom is a sharp ‘zing’ through the tooth when chewing that goes away almost immediately. (CTS)6https://www.sciencedirect.com/science/article/abs/pii/S0022391314000353
- Sporadic sensitivity when biting
- Hot and cold sensitivity
- If a crown feels loose
- A chipped crown
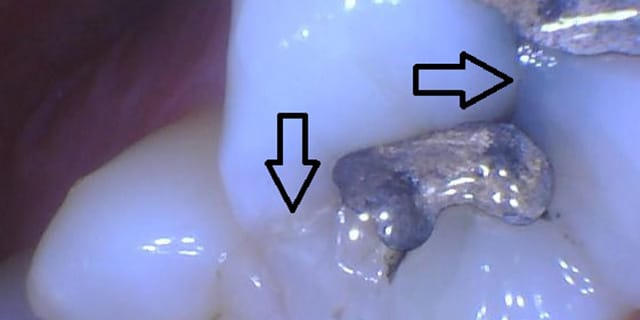
When either the tooth or filling fractures and is still save-able, most often the treatment is a dental crown. Cracked tooth syndrome is an incomplete fracture extending to the dentinThe layer of tooth between the enamel and pulp chamber. and occasionally into the pulpThe nerve tissue of the tooth. of a vital tooth. The classic symptom of CTS is sharp, fleeting pain while either placing or releasing pressure on a tooth, typically induced when eating. The pain immediately dissipates once the tooth is no longer under function.
A dentist will test this by having a patient bite on an instrument called a Tooth Slooth. CTS needs to be resolved immediately by removing the fracture and placing a dental crown on the tooth. This treatment can be unpredictable as it is difficult to tell how extensive the fracture is as it typically doesn’t show up on any type of imaging. Attempting to save the tooth with a crown will give it the best chance of survival.
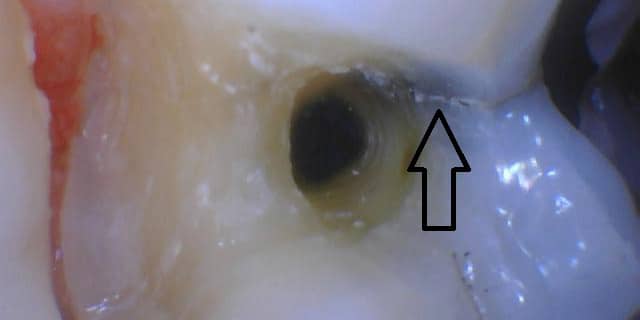
Heat and cold sensitivity is another symptom that may mean a crown is needed. This symptom can indicate many things, one of which is increased wear and tear. It can happen on front or back teeth and if the cold sensitivity is extreme, you will want to call the dentist’s office immediately.
Can I Re-Use My Old Crown?
When an existing has a loose crown, a new crown may not be necessary. It depends on why the crown is loose. The crown can feel loose in many scenarios including when using dental floss or eating. If the dental crown falls off the tooth, it may be reused but only the crown fell off due to cement failure.
When Do I Need to Have an Existing Crown Replaced?
The most common reason to replace an existing crown is when there is recurrent decay. While the gap in margins are minute, as small as 48 ±25 μm when using a digital approach6, a gap still exists. That gap is susceptible to streptococcus mutans, the primary culprit of dental decay7https://www.ncbi.nlm.nih.gov/books/NBK8259/.
One of the most common areas for recurrent decay to occur is the interproximal margin of crowns. When decay forms here, the entire crown must be removed in order to gain adequate access to remove the decay and re-establish a new margin with a new dental crown. The decay should be addressed quickly so it doesn’t affect adjacent teeth.
Can I Fix a Crown With a Filling?
When minor decay forms on the buccalThe same surface as ‘facial’ but technically only on posterior teeth. or lingual margin, it may be able to be fixed with a ‘crown patch’ which is essentially a filling along the margin. Since a crown patch typically goes underneath the crown, the decay must be minor to ensure it is entirely removed. Should the decay extend close to the pulp or apically to the bone, the decay cannot be repaired with a simple filling.
The reason a crown patch cannot be done on interproximal recurrent decay is because of access. Quality dentistry must always be rendered to ensure esthetic, pain free, biologic and longevity in all dental restorations. Dentistry should essentially look and feel like nothing was done. All porcelain crowns, particularly lithium disilicate and zirconia crowns, are especially strong while retaining the natural tooth color.
What Happens During a Crown Procedure?
A dental crown involves a few steps and typically two appointments. At the first appointment, the tooth or teeth are thoroughly anesthetized with local anesthetic. An impression of the tooth and adjacent teeth in its current state is taken. This mold is used to make a temporary crown to sit on the trimmed tooth while the permanent crown is being made in a dental laboratory.
However there are some types of dental crowns that do not require a temporary crown. These exceptions are crowns made using computer aided design computer aided milling technology (CADCAMAn acronym for ‘computer aided design computer aided milling’. This technology digitally designs and makes crowns out of various, large blocks of porcelain.), also known as single day crowns.
The tooth is then prepared by removing any diseased or weak parts of the tooth. These parts are removed with a high speed handpiece and dental burPaired with various types of handpieces, a bur is often referred to as the drill bit. It spins at varying RPMs to cut and shape hard and soft tissue as well as dental materials.. If there are any old restorations that remain, they are often removed and replaced. A build up is commonly placed in the same fashion as seen in regular fillings. If the buildup material is amalgam, the material needs time – at least a full day, to set up before proceeding. If the buildup material is a compositeA synthetic resin that is used for while fillings. This is what most people receive when they get fillings., the tooth can immediately be prepared for a crown.
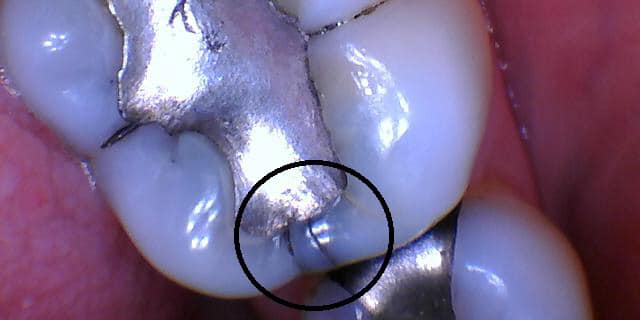
The tooth is then shaved down 1-3 millimeters circumferentially with specific angles to increase mechanical retention of the dental crown. The margin is then shaped appropriately to the type of crown that is being made. A broad generalization is ceramic crowns need to be more uniformly thick, as a thin part will fracture easily. If the ceramic fractures at the margin, it will lead to recurrent decay. This is not the case for metal, as metal can still be strong and metal crowns rarely chip.
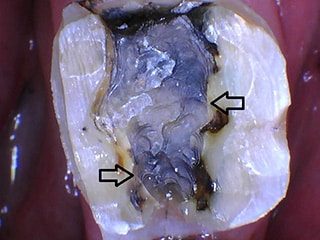
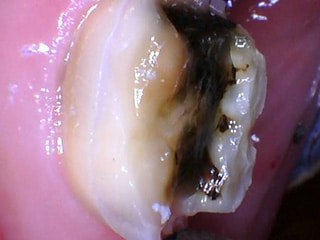
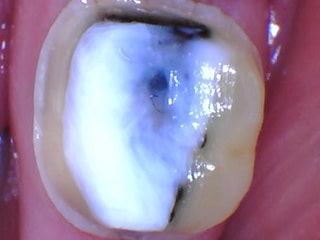
Once the tooth is prepared, an impression of the prepared tooth is made either digitally or with impression material material, with the most common being polyvinyl siloxane (PVS). Sometimes cordA small piece of string that is placed between the teeth and gums (while numbed) to push the gums away from the tooth. is packed into the gingival sulcus which pushes the gum tissue away from the tooth in order to get a better impression of the tooth. Both are extremely accurate and are able to not only replicate the patient’s anatomy, but also the bite.
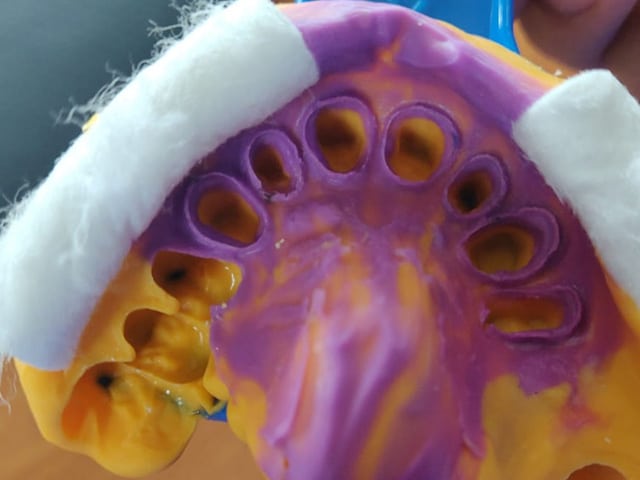
Then a temporary crown is made using the mold taken at the beginning of the appointment. Temporary crowns are made of various materials, such as polymethyl methacrylate [PMMA] or bis-acryl resin. Bis-acryl resin is widely used due to its ability to be easily repaired with flowable composite resin5https://pubmed.ncbi.nlm.nih.gov/15523341/. Once the temporary crown is made, it is fitted to the tooth and cemented with a temporary cement. Then the first appointment is done!
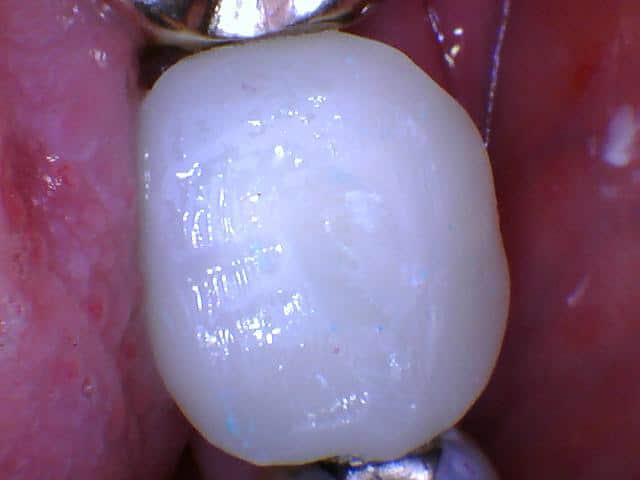
Ideally the tooth would be free of gum disease, especially the front teeth for best esthetics. Even all-porcelain crowns will look bad if the margin is visible, which can appear after treating the tooth for periodontal disease.
The impression of the prepared tooth is sent to a dental lab, which is sometimes inside the dental office itself. The dental lab then makes the crown via different techniques, depending on which types of dental crowns are needed. Gold crowns are typically made via the lost wax casting techniqueA technique that injects a molten gold alloy into a space in the exact shape of a gold crown. This technique is only used with making gold crowns or bridges. and ceramic crowns are milled or stacked for instance. Once the crown is made, it is shipped back to the office which has a typical turnaround time of two weeks. This turnaround time can actually be made shorter with a digital impression.
The second appointment is much faster and easier. Many times the patient doesn’t even need local anesthetic. The temporary crown is removed and the final crown is fitted. The contacts is checked to ensure it isn’t too tight to allow for proper dental flossing. Then the margin is checked to make sure the crown is closed and smooth. The dentist may also take a radiograph is taken to ensure that the margin interproximally is closed. The occlusion (bite) is also checked with articulating paperThin paper that makes marks on teeth when someone bites or chews on it. to make sure the crown isn’t too high. Once the crown passes all the quality control checks, it is cleaned and cemented onto the tooth. After the cement hardens, the excess is removed and you’re free to go!
What Are Some Complications That Can Occur With a Dental Crown?
Dental crowns are an extremely predictable procedure that have few severe complications. When complications do occur, the most common is irreversible pulpitisA condition where the nerve is inflamed and that, as the name implies, is irreversible. When this occurs, the nerve must be removed either by extraction or a root canal. due to excessive irritation to the pulp. When this occurs, the nerve tissue must be removed via a root canal. If left untreated, the pulp will die and cause a periapical abscessA potentially life threatening infection, typically due to a dead nerve, cracked root, or periodontal problem.. Other complications include:
- High occlusion (bite) which can lead to traumatic occlusion. This can cause pain to crowned tooth or opposing teeth, mobility, and TMJ pain8https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3110471/.
- Improper occlusion which can lead to drifting teeth which subsequently leads to an open contactThere is a gap, as small as fractions of a millimeter, between two teeth. This results in significant food impaction and subsequent problems. and food impaction.
- Poor esthetic outcome due to mismatched shade or poor contouring. It should be known that a single anterior crown is extremely difficult to completely match to the adjacent teeth.
- Soreness in the teeth and gums typically occur, but typically subside after a few days.
You will want to call your dentist immediately if you have extreme cold sensitivity that lingers for over 10 seconds. This is a sign of irreversible pulpitis that needs to be diagnosed and treated. Rest assured this is not very common.
How Much Does a Dental Crown Typically Cost?
While the cost will vary on several factors, a general range for the fee for service cost is $600-$3,000. Dental crowns cost will vary if additional procedures are needed. Buildups are the most common procedure paired with crowns. While buildups are not always needed, they are frequently required because crowns are placed on teeth that are missing significant amounts of tooth structure. The fillings under crowns are often old, leaking and the underlying tooth needs to be clean and solid before a crown can be permanently cemented.
The cost of a dental crown is affected by a few things:
- Type of crown
- Insurance coverage
- Service completed by specialist or general dentist
Type of Crown
The type of crown affects the cost. Crowns have different costs to make by the lab, which in turn can make the crown more expensive to the patient. For instance, as the cost of gold rises, the cost of gold crowns will increase. Additionally, esthetic anterior crowns are more technically difficult to make, so they can be more expensive.
Insurance Coverage
Dental insurance can often reduce the total out of pocket cost for patients. When they are a covered benefit, crowns are most commonly covered at 50% of the in-network cost. For example, if the insurance contracted rate is $1,100, the crown will be a total $550 out of pocket cost to the patient. Keep in mind there are factors that will determine insurance coverage and whether or not the service will be covered and how much it will be covered.
Service Provider
As a general rule of thumb, specialists are more expensive than their general practitioner counterparts. This is due to their increased training as well as the fact that the given procedure is the only category of treatment they render. For instance, it is unlikely a dental anesthesiologist will place your implants or complete advanced bone grafting.
If you have any questions about insurance coverage, call your dentist’s office for more clarification.
Frequently Asked Questions About Crowns
For most people, there will be some amount of soreness and discomfort after any treatment is done. However crowns are rarely debilitating and the soreness goes away within a few days, often sooner. Rarely, crowns need additional treatment when complications occur.
As a rule of thumb, crowns have a life expectancy of 10-15 years. Studies have shown that ceramic crowns can last anywhere from 3 to 18 years9https://www.sciencedirect.com/science/article/abs/pii/S030057121630166X while gold crowns can last up to 40 years.
While this varies from office to office as well as the type of crown being made, expect the first appointment to take anywhere from 60 to 120 minutes. The actual treatment time is much less, sometimes as short as 10 minutes. The second appointment is much shorter and takes anywhere from 30 to 60 minutes. A single day crown takes a few more hours to allow time for the crown to be made immediately.
Yes, crowns are permanent. However, like almost all health care treatments, they do not last forever. Comparatively, dental implants are one of the few treatments that have the potential to outlive you.
Was this post helpful?
References
- 1
- 2
- 3
- 4
- 6
- 7
- 5
- 8
- 9