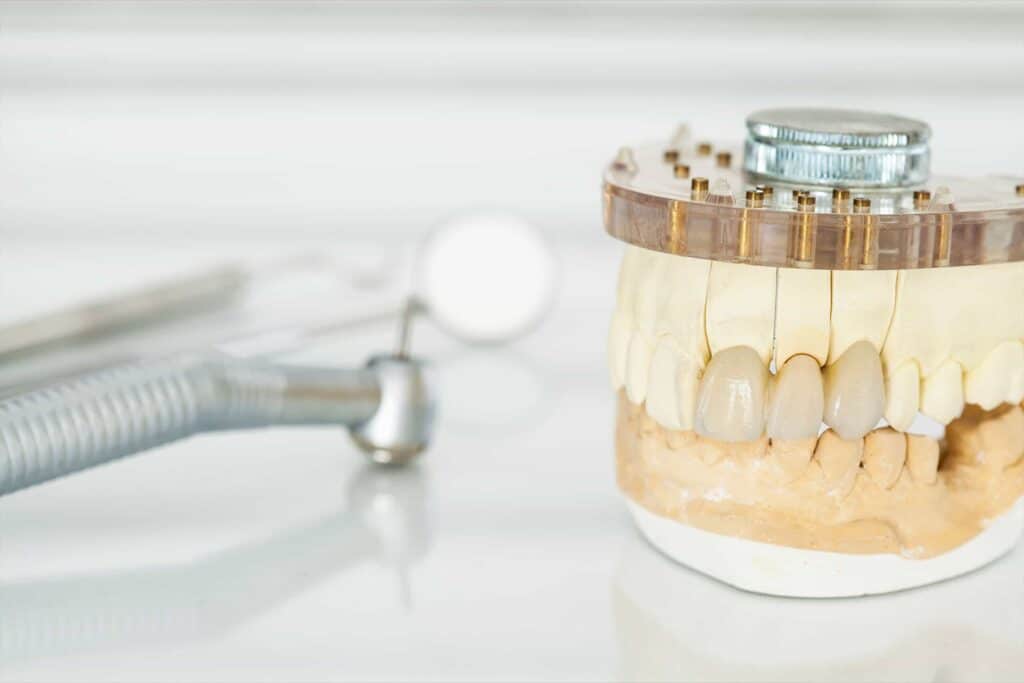
Surface Topography-Adaptive Robotic Superstructures for Biofilm Removal and Pathogen Detection on Human Teeth
Article Link: https://pubs.acs.org/doi/10.1021/acsnano.2c01950
This is a super fascinating article that utilizes cutting edge technology for basic oral hygiene. Every day hygiene targets the removal of a biofilm that forms quickly after removal. This biofilm is composed of microbial cells intertwined with an extracellular matrix and can adhere to numerous surfaces. This is a fancy way of saying that intraorally bacteria produce a very sticky film that attaches onto teeth. And also acts as an anchor to multiply. If not removed regularly, the bacterial by-products end up eroding away the teeth, which is how cavities are formed.
The authors proposed using what they’ve termed “surface topography-adaptive robotic superstructures” (STARS) as a means to improve oral hygiene. The basic principle is to utilize a microrobotic system of iron oxide nanoparticles (IONP). These nanoparticles have unique catalytic and magnetic properties. Through using electromagnetic energy, this system is able to manipulate the IONPs into numerous formations. This occurs by extending and retracting IONPs in micro to centimeter scales. This movement has antimicrobial effects and is able to effectively remove the biofilm layer. Even more fascinating is the adaptability of the IONPs, which are able to get into oddly shaped and hard to reach areas.
While it appears there is a long way to go prior to commercialization of this technology, it has high potential. I believe that this would be game changing in daily hygiene. Especially for those who have limited manual dexterity such as the disabled or elderly. This could be an easy way for them to regularly clean their teeth. If the technology could be refined to also remove calculus or go under the gums, it has huge potential for use in a dental office. It could even be a way for those who have a hard time brushing to easily clean their teeth. Personally I am very interested to see how this technology advances due to it’s incredible versatility.
Smoking as a Risk Factor for Dry Socket: A Systematic Review
Article Link: https://www.mdpi.com/2304-6767/10/7/121
Exodontia or tooth extractions are a very common dental procedure. Teeth are removed for multiple reasons, ranging from advanced decay or periodontal disease, to trauma, or orthodontics. As with all procedures, there are many risks with dental extractions. The most common is a dry socket. A dry socket is when the blood clot that forms in the bone where the tooth was removed is dislodged either fully or partially. This leads to extreme pain, halitosis or bad breath, decayed debris and requires professional intervention for relief. When faced with this reality, prevention is a superior option but can be difficult for some, particularly smokers.
The adverse effects of smoking are well documented and generally known. The oral cavity is equally susceptible to disease such as staining, bad breath and periodontal disease. During the healing period after extractions, smoking increases the odds of a dry socket. In this study tobacco use increased the odds of dry sockets to a staggering 58% over 6.8% in overall patients.
The authors didn’t heavily discuss vaping or electronic cigarettes. However another study within this systematic review found that e-cigarettes are thought to be less harmful to oral health. I would like to have seen both e-cigarettes and marijuana cigarettes focused on more due to their current relevance. However I understand the difficulty of studies with marijuana due to differences between state and federal regulations. A good thought until shown otherwise is to categorize e-cigarettes and marijuana cigarettes the same as tobacco cigarettes. My advice would be to avoid them after dental extractions to avoid complications.
Association between Periodontitis and COVID-19 Based on Severity Scores of HRCT Chest Scans
Article Link: https://www.mdpi.com/2304-6767/10/6/106
COVID-19 has been a disease of interest for some time now and there are established risk factors that can affect the severity of someone infected with the coronavirus. These include age, sex, BMI, smoking status and general health status, which includes diabetes, high blood pressure and lung diseases to name a few. The purpose of this study was aimed at determining the relationship between periodontal disease as a risk factor in COVID-19.
294 patients had a combination of mild, moderate and severe COVID-19 symptoms. Some findings were consistent with previous beliefs such as patients with severe COVID-19 had a higher BMI, were older, and had other chronic health issues including diabetes than those with less severe COVID-19 symptoms. Additionally significantly more patients with mild COVID-19 symptoms cleaned their teeth twice daily than those with more severe COVID-19. Additionally they found that the group with severe COVID-19 had a significantly higher number of individuals with periodontitis (87.5%) than the other two groups.
The researchers were able to determine that there is a significant association between periodontitis and severe COVID-19 infections. Periodontitis may play a role on the course and outcome of those infected with COVID-19. One theory is that the presence of increased intraoral bacteria may increase the amount of aspirated bacteria resulting in worsening symptoms due to COVID-19’s affect on the lungs. The researchers concluded that evaluation of the periodontal status should be a part of the COVID-19 treatment protocol as it may be a risk factor for severe COVID-19.
Pilot Study of a New Mandibular Advancement Device
Article Link: https://www.mdpi.com/2304-6767/10/6/99
Obstructive sleep apnea (OSA) is prevalent amongst many adults and often goes undiagnosed and untreated. The current mainstream forms of interventive treatment includes a continuous positive airway pressure (CPAP) machine or a mandibular advancement device (MAD). The latter uses a device that is worn and anchored on the teeth which brings the mandible forward and increases the airway space. This reduces or eliminates the collapse of the soft tissues during sleep, which is the primary cause of OSA.
This study aimed to determine the effectiveness of a new type of MAD. Typically MADs are made of a combination of acrylic and metal to treat OSA. This MAD in question is called the NOA by OrthoApnea which is a 3D printed device. For 3 months, several patients with mild, moderate, and severe OSA were treated with this new style of MAD. They determined that it was effective in reducing the number of events in which the patient stopped or had reduced breathing at night. It was even effective in treating severe cases, which should be treated with a CPAP by the gold standard. However due to the low compliance of CPAP, the authors determined that this fully custom style of MAD may be a good alternative treatment option for those suffering from OSA.